A Systematic Review of Stroke Recognition Instruments in Hospital and Prehospital Settings
Originals
Nursing triage in acute stroke
Araceli Rodríguez Vico1 , Fernando Sánchez Hernández2
1. Graduada en Enfermería. Servicio de Urgencias. Hospital Universitario de Salamanca. Profesora Asociada. Facultad de Enfermería y Fisioterapia. Universidad de Salamanca. España. arvico@usal.es
2 . Médico Urgenciólogo. Profesor Titular de Universidad. Facultad de Enfermería y Fisioterapia. Universidad de Salamanca. España.
Abstract:
In recent decades, the office of nursing in triage and screening of patients in emergency services, both in prehospital environs and specially in hospitals, is essential and indisputable. In order to analyze the triage carried out past nursing to find patients with astute stroke, and if necessary better it, a retrospective study was carried out of the cardinal presentations of stroke, the calibration of the National Plant of Health of the U.s., and the modified Rankin scale, practical in the nursing triage set up at the Salamanca University Infirmary, during the catamenia between 2016 and 2019, both inclusive. The full number of clinical records analyzed was 1572. The analysis is focused on the reliability, evaluated by nursing, of the cardinal presentations of acute stroke, and of the two scales, compared to the traditional rapid algorithms for stroke detection, in particular the FAST method, and the Cincinnati scale. Our study shows that there are several clinical presentations that escape the rapid scales, and so information technology is essential to expand the triage methods of acute stroke carried out by nursing, in social club to avoid delays in detection and definitive treatment (fourth dimension-dependent affliction). Thus, the expanded identification of cardinal presentations, together with the use of more detailed scales practical by trained nurses, appear to be very useful tools for the detection of astute stroke.
Key words:Stroke; triage; key presentation; nursing
INTRODUCTION
Triage is the first contact of the patient, the family, and the caregivers, with the health professional, both at the pre-hospital and hospital levels1. Triage methods are rapid scales and protocols intended to classify and prioritize patients in need of urgent care. Morbidity and mortality can exist prevented if patients are chop-chop classified and treated efficiently, since many deaths occur inside the first hours of admission2. With a precise triage organisation, carried out by trained people, and with adequate algorithms, the incidence of adverse events decreases significantly, especially in time-dependent diseases. If the triage is well carried out by appropriate health professionals, it is a key tool in the nomenclature and prioritization of emergency treatment in the infirmary setting, every bit well as in the criteria for pre-hospital and inter-hospital emergency transport3 , four.
In most hospital triage areas, the nurse is the showtime clinically trained wellness professional who will assess the clinical situation of patients. He must detect the nearly important clinical data, and determine if the patient should be treated immediately, or if the pathology is not unsafe to life, and can wait a reasonable fourth dimension. Therefore, its principal objective is that patients can exist, as shortly as possible, selected, classified, treated, or discharged in a timely wayiv )( 5 )( 6.
Considered as blueish codes, fourth dimension-dependent pathologies, such as acute stroke, acute coronary syndrome, or severe trauma, cannot exist delayed under any circumstances, and must exist discovered immediately through correct triage. Acute stroke is a serious, life-threatening clinical emergency condition that requires immediate detection and treatment (the faster treatment is received, the less harm and injury the patient suffers). Patients with astute stroke are therefore normally evaluated for the first time in hospitals, by nurses responsible for the triage area. Different studies have clearly demonstrated the effectiveness of triage protocols for this pathology in reducing the time from the patient entering the infirmary to the final specific handling 7 , viii.
For many years now, different methods have been used to correctly triage stroke, both at the pre-hospital and hospital level. The FAST (Face/Arm/Spoken communication/Time) and FASTER (Face/Arm/Stability/Optics/React) methods and the Cincinnati scale (Facial droop/Arm drift/Speech) are iii of the most common. However, these simple methods may be totally insufficient in a nursing triage expanse 9 )( 10 )( eleven )( 12 with a potential gamble of error and delay in diagnosis, when the cardinal presentation is non so typical to exist framed in these methods.
Based on the above, the objective of the present study is to carry out a retrospective analysis of the central presentations of acute stroke detected in the infirmary triage area by the nursing professional person, together with the immediate application of the NIHSS13 (National Institute of Health Stroke Calibration) and MRSfourteen (Modified Rankin Scale) scales, at the University Hospital of Salamanca, during the period between 2016 and 2019.
Material AND METHODS
In this study nosotros have analyzed a total of 2080 medical records of patients with confirmed astute stroke. The patients correspond to the surface area of influence of the Salamanca University Hospital (including the 112 Emergency Service), during the period from 2016 to 2019, both inclusive. The information of the patients was obtained from the medical records under the strict command and supervision of the Documentation Service of the University Hospital of Salamanca. Data direction was carried out under the rules of the Ideals Committee for the use of the information collected in the patients' medical records.
Iii groups of information were analyzed: the cardinal presentations, and the NIHSS and MRS scales. Some clinical records did non comprise all the information under study or were not clearly specified. When information technology afflicted two of them, they were discarded. Nigh of the fourth dimension they were due to the absenteeism of the NIHSS score forth with the MRS. Thus, the final number of stories analyzed in the iv years was 1572 (2016: 375. 2017: 371. 2018: 421. 2019: 405.)
Table 1: Cardinal presentations

The cardinal presentations were divided into ten different groups, in social club to accept an like shooting fish in a barrel to use, but expanded method of detecting possible presentations, both typical and less frequent, equally shown in Tabular array 1.
The NIHSS scale was always performed subsequently rapid triage of cardinal presentations, during the flow in the emergency department prior to computed tomography. NIHSS includes different items, as specified in Table ii. Each item is scored from 0 to 2, 0 to three, or 0 to 4 points. The total score ranges from 0 to 42 (the higher the score, the more severe the stroke). The original NIHSS13 calibration (Tabular array two) has been applied to our report, every bit it is the virtually widely used, although there are several versions bachelor (NIHSS with five, 8 and xi items).
Tabular array 2: NIHSS Calibration

MRS14 is a 6-signal disability scale with possible scores ranging from 0 to five. Typically, a split up category is added for patients who die (half-dozen). Although there are different versions of the Rankin scale, for our study we have used the most widely used modified version in emergency departments and neurology (Table three).
Table 3: MRS Calibration

RESULTS
In the distribution by gender, nosotros found a slight predominance of male person patients (871), compared to female (701), which represents 55.forty%, compared to 44.sixty%. A total of lxx patients were in the grouping under fifty years of age. The grouping with the highest number was that of l to 80 years with a total of 908, with 594 patients existence within the group of more than than fourscore years. In pct they represent 4.46%, 57.76% and 37.78% respectively.
Analyzing the cardinal presentations (Prototype 1), the clinical data with the highest expression were language disorders with a total of 285 patients (18.xiii%). The way of describing them by relatives and caregivers was very diverse, including expressions such equally "He does not speak", "It is hard for him to speak", "He is non understood", and "He speaks strangely".
In the ataxia group all gait disturbances / difficulties were included, every bit well as falls, both at home and on public roads. A total of 240 patients (15.26%) presented this cardinal presentation.
Paresis (231, 14.69%) and plejia (189, 12.02%), ranked fourth and fifth respectively. They were referred to every bit "Difficulty moving a limb", "Weakness of a limb", "Not moving a limb", etc.
Facial asymmetry, accounted for a full of 139 cases (8.84%). Referred to in a very typical mode with expressions such as "His mouth has been twisted" or "One side of his oral cavity has fallen off".
Behavioral alteration was the fundamental presentation in 7.44% of all cases, bold 117 patients in absolute numbers. Information technology should be noted that although in some cases the beliefs modification was axiomatic, in others it was subtle changes, often habit changes, sudden changes in character, fifty-fifty mood furnishings.

Image 1: Key presentations (Results)
Headache, be information technology holocranial, hemicranial or regional, stood out as the onset in 56 cases (iii.56%). It was observed in several cases, after imaging diagnosis, that the location of the hurting referred by the patient had a clear relationship with the afflicted vascular territory. The least frequent cardinal presentation detected in this report was ocular alterations with a total of 31 cases (ane.97%). The most frequent clinical finding in this grouping was diplopia.
Finally, in some histories the onset symptoms were non conspicuously divers, or presented other forms, corresponding more to other underlying pathologies or epiphenomena, than to clinical information related to stroke.
Considering the NIHSS calibration, the most of import number of patients was in the range between 12-xv points, with a total of 474 cases (30.15%), closely followed by the range between 16-twenty points, with a full of 435 patients (27.67%).
87 patients (24.62%) were located in the group between 7 and 11 points, while 186 (eleven.83) were located in the area with the highest score, above 20 points. With less than 7 points, a total of 36 patients (2.29%) and the grouping of histories in which the NIHSS were non explicitly recorded at the beginning of the image (64, four.07%).

Epitome ii: NIHSS Scale (Results)
Finally, analyzing the MRS, the most important grouping of patients presented 0 points, beingness a total of 808 (51.40%), which indicates that their previous baseline status allowed them to be valid for all possible activities of daily life.
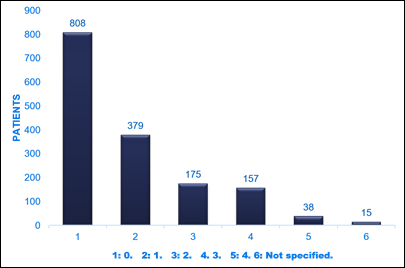
Image three: MRS Scale (Results)
The adjacent 2 groups with the highest number of patients were those with a score of 1 (379, 24.11%) or 2 points (11.13%). 157 patients (9.99%) had a total of three points at the time of stroke diagnosis and 38 patients (2417%) added iv points.
It should be noted that there were no cases of patients with 5 or vi points, which is totally logical given that it would mean a previous maximum disability (5 points) or a previous expiry (6 points) and that in 15 patients (0.95%), MRS was non indicated.
DISCUSSION
Classification and triage by nurses and other health professionals, both at the prehospital and infirmary level, is a complicated method/technique, as it is sometimes performed in a difficult and adverse surroundings. The emergency services are frequently overwhelmed by the huge number of patients demanding clinical care equally quickly equally possible. In response to these special weather condition, many studies take demonstrated the efficiency of the nursing triage procedure. Nursing triage is an effective intervention to detect life-threatening diseases, specially time-dependent ones. In a triage environment, nurses must manage advisable algorithms/scales to detect these dangerous states of patients15 )( 16 )( 17 )( 18 )( 19.
Acute stroke is the second leading cause of death worldwide and i of the leading causes of disability, with an increasing incidence in developed countries. Ischemic stroke caused by arterial occlusion is responsible for most cerebrovascular accidents (more 70%). Since it is a time-dependent situation, the right direction must include a rapid and precise triage and diagnosis, to attain, if necessary, reperfusion of the ischemic encephalon area with intravenous thrombolysis and / or endovascular thrombectomytwenty.
Simple traditional stroke triage methods are useful tools to hands detect acute stroke (very few particular scales). They include the FAST and FASTER algorithms, and some scales such as the Cincinnati scale. They are widely used especially past pre-hospital emergency services, equally they are easy and quick to learn or perform and have a good ability to place potential stroke patients. However, it only evaluates the presence of some symptoms (facial paralysis, upper limb weakness and voice communication disturbances), but does non evaluate other less frequent cardinal presentations, and the severity of the stroke21. Therefore, the use of scales and methods with greater sensitivity in the detection of patients with acute stroke in triage sets becomes essential.
The NIHSS scale is a systematic evaluation tool, valid for detecting acute stroke, measuring its severity, guiding the advisable handling, and predicting the patient's upshot13. Furthermore, it provides a common language for the commutation of data amongst healthcare professionals. The NIHSS scale is quick and easy to administrate by trained professionals (5-7 minutes) and requires minimal equipment. There are much more circuitous methods to handle big volumes of different clinical data, but they are not suitable for use in triage emergency services due to their complexity22 , 23 ) being reserved more for intensive intendance units.
The MRS calibration is oftentimes used in astute strokes to detect the patient'due south previous land and the afterward state at the time of leaving the hospital, but also to select which patients should or should not be treated. It is a coded scale from 0 (no symptoms) to 5 (severe inability) and half-dozen (death). The MRS scale in stroke/triage trials can divide patients into ii groups: Scores from 0 to 2/3 are positive for specific treatments such as endovascular (if they meet the residuum of the requirements). Still, the rest of the scores (>three) are divers as negative for this type of treatment. A limitation of this scale has been the subjective conclusion between categories and the reproducibility of the score by examiners and patients.
As observed in our written report through the analysis of cardinal presentation, there are multiple forms of presentation of acute stroke. Several of them, the most frequent, would exist easily framed and detectable, using the traditional FAST/FASTER methods and the Cincinnati scale, but other presentations clearly escape these rules. Presentations such equally decreased level of consciousness (fifteen.84%), behavioral disturbances (vii.40%), headache (iii.56%), and ocular disturbances (1.90%) are not considered in them and represent a full of 27% of the presentations. If they are considered, it may exist that they delay the diagnosis, escaping the initial detection in a triage room, with the serious consequences that this can have.
In other words, more than 25% of strokes may go undetected in the triage room if unproblematic and excessively rapid triage scales are followed. Therefore, the utilize of extended cardinal presentation triage schemes should be an essential tool, as shown in Table i. In this sense, the use of more complete scales such us NIHSS by trained nurses becomes essential. Forth with this, every bit an essential complement to rapid screening for firsthand treatment, the application of the MRS calibration should be required in the triage area equally a fundamental tool for the selection of patients who should receive immediate treatment and which should not.
Thus, the feel and skills of nursing professionals24 )( 25 )( 26 )( 27, the combination of a selective search for central presentations with a selected group of symptoms, together with the NIHSS and MRS scales, constitute useful tools for screening and the correct diagnosis of acute stroke. The fundamental part of nursing professionals becomes key in the present and in the firsthand future of hospital triage, and must be considered in all emergency services.
CONCLUSIONS
In the calorie-free of our results, the specific role that nursing plays in the triage room in general, and in the detection of fourth dimension-dependent diseases, with special mention of acute stroke, is crucial. Given that more than 25% of acute stroke presentations are not typical, the nursing professionals should reinforce their specific preparation in the extended triage scales and less frequent presentations of this time-dependent disease.
REFERENCIAS
ane. Wolf LA, Delao AM, Perhats C, Moon MD, Zavotsky KE. Triaging the Emergency Department, Not the Patient: United States Emergency Nurses' Experience of the Triage Process. J Emerg Nurs. 2018; 44(iii): 258-66. DOI: 10.1016/j.jen.2017.06.010. [ Links ]
2. Bazyar J, Farrokhi M, Salari A, Khankeh Hour. The principles of triage in emergencies and disasters: a systematic review. Prehosp Disaster Med. 2020; 35(3): 305-313. DOI: 10.1017/S1049023X20000291. [ Links ]
3. P. Funderburke, P. Exploring best practise for triage. J Emerg Nurs. 2008; 34(2): 180-182. DOI: ten.1016/j.jen.2007.11.013. [ Links ]
iv. Haghigh Southward, Ashrafizadeh H, Mojaddami F, Kord B. A survey on knowledge level of the nurses about hospital Triage. J Nurs Educ. 2017; v (six): 46-52. DOI: 10.21859/jne-05067. [ Links ]
5. Magnusson C, Herlitz J, Axelsson C. Affiliations expand Pre-hospital triage operation and emergency medical services nurse's field assessment in an unselected patient population attended to past the emergency medical services: a prospective observational study. Scand J Trauma Resusc Emerg Med. 2020; 28(one): 81. DOI: 10.1186/s13049-020-00766-1. [ Links ]
6. Reisi Z, Saberipour B, Adienh Thousand, Hemmatipour A, Shahvali Due east.A. The level of sensation of the emergency department nurses of the triage principles in teaching hospitals. J of Nurs Mid Sci. 2018; 5 (1): 32-37. DOI: x.4103/JNMS.JNMS_5_18 [ Links ]
7. William J. Powers, Alejandro A. Rabinstein, Teri Ackerson, Opeolu M. Adeoye, Nicholas C. Bambakidis, Kyra Becker, José Biller, Michael Brown, Bart M. Demaerschalk, Brian Hoh, Edward C. Jauch, Chelsea S. Kidwell, Thabele Yard. Leslie-Mazwi, Bruce Ovbiagele, Phillip A. Scott, Kevin N. Sheth, Andrew M. Southerland, Deborah V. Summers, and David L. Tirschwell and on behalf of the American Heart Clan Stroke Quango. 2018 Guidelines for the Early Management of Patients With Astute Ischemic Stroke: A Guideline for Healthcare Professionals From the American Heart Association/American Stroke Association. Stroke. 2018; 49: e46-e99. DOI: x.1161/STR.0000000000000158. [ Links ]
8. Ekundayo OJ, Saver JL, Fonarow GC, Schwamm LH, Xian Y, Zhao 10, Hernandez AF, Peterson ED, Cheng EM. Patterns of emergency medical services use and its association with timely stroke treatment: findings from Become With The Guidelines-Stroke. Circ Cardiovasc Qual Outcomes. 2013; 6: 262-269. DOI: ten.1161/CIRCOUTCOMES.113.000089. [ Links ]
nine. BE-FAST (Balance, Optics, Face up, Arm, Speech, Fourth dimension) Reducing the Proportion of Strokes Missed Using the FAST Mnemonic Aroor SS, Singh R, Goldstein LB, Stroke. 2017; 48: 479-481. DOI: 10.1161/STROKEAHA.116.015169. [ Links ]
10. Rudd M, Buck D, Ford GA, Price CI. A systematic review of stroke recognition instruments in hospital and prehospital settings. Emerg Med J, 2016; 33(11): 818-822. DOI: 10.1136/emermed-2015-205197. [ Links ]
xi. Schlemm East, Ebinger G, Nolte CH, Endres M, Schlemm L. Optimal transport destination for ischemic stroke patients with unknown vessel status: use of prehospital triage scores. Stroke. 2017; 48: 2184-2191. DOI: x.1161/STROKEAHA.117.017281. [ Links ]
12. Venema East, Lingsma HF, Chalos V, Mulder M, Lahr MMH, van der Lugt A, van Es A, Steyerberg EW, Hunink MGM, Dippel DWJ, Rozemberg B. Personalized prehospital triage in astute ischemic stroke. Stroke. 2019; 50: 313-320. DOI: 10.1161/STROKEAHA.118.022562. [ Links ]
xiii. Williams LS, Yilmaz EY, Lopez-Yunez AM. Retrospective Assessment of Initial Stroke Severity with the NIH Stroke Scale Stroke. 2000; 31: 858-862. DOI: 10.1161/01.STR.31.4.858 [ Links ]
14. Banks JL, and Marotta CA. Outcomes Validity and Reliability of the Modified Rankin Scale: Implications for Stroke Clinical Trials A Literature Review and Synthesis. Stroke. 2007; 38: 1091-1096. DOI/10.1161/01.STR.0000258355.23810.c6. [ Links ]
15. Stanfield LM. Clinical determination making in triage: an integrative review. J Emerg Nurs. 2015; 41(5): 396-403. DOI: ten.1016/j.jen.2015.02.003. [ Links ]
16. Delmas, P, Fiorentino A, Antonini M, Vuilleumier S, Stotzer G, Kollbrunner A, Jaccard D, Hulas J, Rutschmann O, Simon J, Hugli O, Keranflec'h CG, Pasquier J. Furnishings of ecology distractors on nurse emergency triage accuracy: a pilot study protocol. Pilot Feasibility Stud. 2020 vi: 171. DOI: 10.1186/s40814-020-00717-eight [ Links ]
17. Chen SS, Chen JC, Ng CJ, Chen PL, Lee PH, Chang WY. Factors that influence the accuracy of triage nurses' judgement in emergency departments. Emerg Med J. 2010; 27(6): 451-455. DOI: x.1136/emj.2008.059311. [ Links ]
xviii. Mistry B, Stewart De Ramirez S, Kelen G, PSK S, Balhara KS, Levin S, et al. Accuracy and Reliability of Emergency Section Triage Using the Emergency Severity Index: An International Multicenter Assessment. Ann Emerg Med. 2018; 71(v): 581-7.e3. DOI: 10.1016/j.annemergmed.2017.09.036. [ Links ]
19. Martin A, Davidson CL, Panik A, Buckenmyer C, Delpais P, Ortiz Thou. An examination of ESI triage scoring accuracy in relationship to ED nursing attitudes and experience. J Emerg Nurs. 2014; 40(5): 461-468. DOI: 10.1016/j.jen.2013.09.009. [ Links ]
20. Smith EE, Kent DM, Bulsara KR, Leung LY, Lichtman JH, Reeves MJ, Towfighi A, Whiteley WN, Zahuranec D. Accuracy of prediction instruments for diagnosing large vessel apoplexy in individuals with suspected stroke: a systematic review for the 2018 guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Center Association/American Stroke Association. Stroke. 2018; 49: e111-e122. DOI: 10.1161/STR. 0000000000000160. [ Links ]
21. Berglund A, Svensson L, Wahlgren N, von Euler Grand; HASTA Collaborators. Face Arm Voice communication Time Test use in the prehospital setting, better in the ambulance than in the emergency medical communication center. Cerebrovasc Dis. 2014; 37: 212-216. DOI: 10.1159/000358116. [ Links ]
22. Sánchez F, Ballesteros, JC, Kraiem MS, Sánchez M, Moreno MN. Using Ensembles and a Clustering-Based Undersampling Approach", Appl. Sci. 2019; 9: 5287. DOI: 10.3390/app9245287 [ Links ]
23. González, J., Martín, F., Sánchez, M., Sánchez, F. and Moreno Yard.N. "Multiclassifier systems for predicting neurological outcome of patients with severe trauma and polytrauma in intensive care units". J Med Syst. 2017; 41:136, DOI: ten.1007/s10916-017-0789-one. [ Links ]
24. Reay G, MacDonald LS, Then KL, Hall G, Rankin JA. Triage emergency nurse determination-making: Incidental findings from a focus group study. Int Emerg. 2020; 48: 100791. DOI: ten.1016/j.ienj.2019.100791. [ Links ]
25. Levin S, Toerper M, Hamrock Due east, Hinson JS, Barnes S, Gardner H, et al. Machine-Learning-Based Electronic triage more than accurately differentiates patients with respect to clinical outcomes compared with the emergency severity index. An Emerg Med. 2018; 71(five): 565-74.e2. DOI: 10.1016/j.annemergmed.2017.08.005. [ Links ]
26. Brosinski CM, Riddell AJ, Valdez Southward. Improving triage accuracy: a staff development arroyo. Clin Nurse Spec. 2017; 31(3): 145-148. DOI: 10.1097/NUR.0000000000000291. [ Links ]
27. Martin A, Davidson CL, Panik A, Buckenmyer C, Delpais P, Ortiz K. An examination of ESI triage scoring accurateness in relationship to ED nursing attitudes and feel. J Emerg Nurs. 2014; forty(5): 461-468. DOI: 10.1016/j.jen.2013.09.009. [ Links ]
 Este es un artículo publicado en acceso abierto bajo una licencia Creative Eatables
Este es un artículo publicado en acceso abierto bajo una licencia Creative Eatables
blackwellacesturod.blogspot.com
Source: https://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S1695-61412021000400108&lng=en&nrm=iso&tlng=en
0 Response to "A Systematic Review of Stroke Recognition Instruments in Hospital and Prehospital Settings"
Enregistrer un commentaire